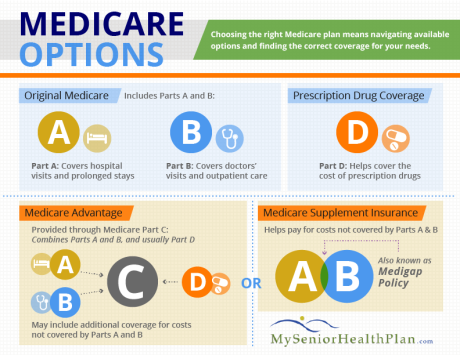
Medicare Parts
So what do all these Parts mean, anyway?
Let’s break it down.
Original Medicare
Original Medicare is the collective name for Medicare Parts A and B.
Part A
Part A is one of the two parts that make up Original
Medicare, and it covers hospital costs. Part A is
available, at no additional cost, to everyone who
qualifies for the Medicare program. Why? Because
you’ve already paid for it! Anyone who has paid
Social Security taxes in the United States pays into
the Medicare program, and the costs of Part A come
out of that money. If you or your spouse has worked
for at least 40 quarters in the U.S., you’re eligible for
Medicare Part A.
In general, Part A covers:
• Hospital care
• Skilled nursing facility care
• Nursing home care
• Hospice
• Home health services
Part B
Medicare Part B, the other part of Original Medicare,
covers services needed to diagnose or treat a medical
condition, illness, or disease. It’s easiest to think about
it as the part that covers your doctor’s visits, although
Part B covers services far beyond simple checkups,
like research, testing, and certain medical equipment.
Medicare Part B also takes care of preventive services
that help you avoid illness or detect it at an early stage
when treatment will work the best.
In general, Part B covers:
• Doctor visits
• Ambulance services
• Durable medical equipment (DME)
• Mental health: inpatient, outpatient, and partial
hospitalization
• Getting a second opinion before surgery
• Limited outpatient prescription drugs
Medicare Part B only covers “medically necessary”
services that have been approved by CMS. Certain
tests, items, or services are covered in all cases; others
vary by your circumstances (see the Appendix). If you
need care that is not considered “medically necessary,”
you may be able to appeal your case to Medicare, so
you should talk to your doctor about further steps.
Part C
Also known as Medicare Advantage, Medicare Part
C is offered by private insurance companies that are
approved by Medicare. It offers the same coverage as
original Medicare, but adds coverage for other services.
These vary widely plan by plan, but they can include:
• Vision
• Hearing
• Dental
• Health and wellness programs
• Prescription drugs
If you’re interested in an all-in-one Medicare Advantage
plan it’s a good idea to talk to one of our licensed
agents about your options. They will include some or
all of these kinds of plans:
Health Maintenance Organization (HMO)
plans
HMOs limit your healthcare options to in-network
providers. Except in an emergency, you can only go to
doctors, other health care providers, or hospitals in
the plan’s network. If you need some particular tests
or care from specialists, you may also need to get a
referral from your primary care provider.
Preferred Provider Organization (PPO) plans
A PPO also limits your provider options, but not as
much. You pay less, sometimes significantly less,
if you use in-network doctors, hospitals, labs, and
other providers. For instance, in-network you may be
responsible for a small copay, while out-of-network you
may need to pay coinsurance, a percentage of your bill
that’s often more than a copay.
Private Fee-for-Service (PFFS) plans
PFFS plans offer wider options. As in Original Medicare,
you can likely go to any provider who agrees to treat
you. However, the amount of the provider’s fee for
which you’re responsible may vary plan to plan.
Special Needs Plans (SNPs)
SNPs are for special groups of people, like those who
have both Medicare and Medicaid, live in a nursing
home, or have certain chronic medical conditions.
HMO Point-of-Service (HMOPOS) plans
These plans are still HMO plans, but they offer broader
options than most. They may allow you to get some
services out-of-network for a higher copayment or
coinsurance.
Medicare Supplement Highlights:
■ Your Medicare Supplement policy enables you to see any doctor or provider who accepts Medicare.
■ Your Medicare Supplement policy covers your health care needs anywhere in the country.
■ Benefits can be paid to you, your doctor or your hospital.
■ Your policy has no Pre-Existing Condition* waiting period. Your coverage begins immediately.
■ Your policy is Guaranteed Renewable for life. As long as you pay your premiums on time.**
■ 30-Day Free Look If you are not totally satisfied, you may return your policy within the first 30 days for a full refund of the premiums you paid.
Exclusions and Limitations: Your Medicare Supplement policy will not pay for:
■ any medical expenses incurred before the effective date of your policy
■ any expenses paid for by Medicare
■ any services for expenses that are not Medicare-approved expenses
How to Pick a Medicare Policy
When you’re picking a Medicare policy, it helps to start
by making a list.
• Write out your current and expected healthcare
needs.
• Write out your habits. For instance, do you travel?
Are you particularly active? Do you smoke?
• Write out your income, and your potential budget
for out-of-pocket expenses.
• Consider your location. Which hospitals and
doctors are most convenient to you?
• Ask your current healthcare providers what type
of coverage they accept. Do you want to keep your
current providers?
As you begin to make your choices, take each of these
factors into account. Then, list in hand, call a licensed
agent. We have a lot of experience in
guiding you through the things you need to think about
in order to select the kind of policy that works for you.
Picking a Medicare policy may seem complicated, but
it’s easier than it sounds. Check out our infographic to
the right to see the steps to take when deciding on a
Medicare policy.
Privacy Notice: By clicking the send button, you agree that we may contact you at the listed phone number to verify your interest in receiving quotes. Receiving quotes through our website is always free and you are under no obligation to purchase any goods or services as a result of this request. Your information will not be passed, and will be kept private. By using this form you agree to the terms of our private policy as so stated.